When COVID-19 hit New Hampshire, nonprofit organizations serving vulnerable people remade programs and the way they are delivered.
People with disabilities are among the most vulnerable. Many have multiple medical conditions that put them at high risk for the coronavirus. Some are flourishing after the nonprofits they trust to keep them healthy, safe or in-touch with their community switched to virtual programs. Some survived as their nonprofit continued in-home visits or 24/7 residential services. Some are struggling as COVID restrictions and other factors limit access to their pre-COVID safety net.
Nonprofits who support those people, already operating on thin margins, have incurred significant additional costs – and in some cases lost revenue – as they have adapted to continue to provide services.
The Charitable Foundation has made grants from its Community Crisis Action Fund and other funds, and released multi-year operating grants early, to support the work of nonprofits that help people with disabilities.
Here are just a few of their stories:
Gateways Community Services
“We reconstructed all of how we deliver services,” said Sandy Pelletier, CEO of Gateways Community Services in Nashua . “We delivered a majority of our services remotely, except for those things that were frontline services for individuals who live in community residences or shared living.”
Gateways serves more than 3,400 people of all ages with disabilities, autism, dementia and chronic illness. It is one of ten “area agencies,” designated in state law as a 24/7, 365-day-a-year safety net organization.
The first dizzying weeks of the pandemic were alarming, Pelletier said, beginning with a phone call on a Friday afternoon saying that when the two dozen clients in their dementia and Alzheimer’s day program based at Alvirne High School went home in the next hour, they would not be able to come back.
“We were told that the school was closing down for students and that we could no longer be in the building,” she said. Gateways tried to continue the services remotely, but because of technology, cognition and other challenges, they could not. They hope to resume in-person services for a smaller number of participants in the fall.
Gateways’ team worked seven days a week for more than two months, implementing ways to respond, safely, to the people they supported, their families and guardians, and Gateways’ 700 employees. The front-line workers who serve people with disabilities do so for modest pay – and the pandemic added an additional layer of risk and stress.
The Gateways team couldn’t deal with one program at a time. All needed attention right away, even as crucial COVID information changed almost daily and the organization’s providers were limited by a lack of protective equipment such as masks and gowns.
Gateways turned to telehealth rather than in-home visits for young children with developmental delays. Staff members also worked from home to continue serving other clients.
It was overwhelming to make sure providers had the laptops, technology and other tools they needed.
Remote services didn’t work well for children with autism, so Gateways safely continued in-person visits for five or six weeks, switched online briefly, then returned to in-person work in early summer.
At the same time, Gateways worked to ensure its most vulnerable clients – those who need 24/7 support – were safe and healthy.
“Some may not understand the disease and protect themselves and may not have the wherewithal or the tools to live in this environment,” Pelletier said. “How were we going to support them?”
Employees’ lives also were upended.
“All of your workforce had to deal with their personal situation, like children not going to school and homeschooling and people were concerned about the spread of this. People in our field were getting infected,” Pelletier said.
Across New Hampshire’s system for caring with people with developmental disabilities, unlike in some states that run large congregate-living facilities, there have not been high rates of COVID-related deaths. But three people in New Hampshire were tragically lost to COVID, including one Gateways client.
Pelletier said cooperation between the state, counterparts in the state and nationwide, the congressional delegation, community donors, federal emergency relief and two grants from Charitable Foundation helped Gateways continue helping its clients.
But she said none of it would have happened without dedicated staff.
“Those individuals who are on the front line every day, working in the community residences or in a day program, are really the heroes,” Pelletier said. “They put their lives on the line in a circumstance where no one could give them a description of how this was going to play out.”
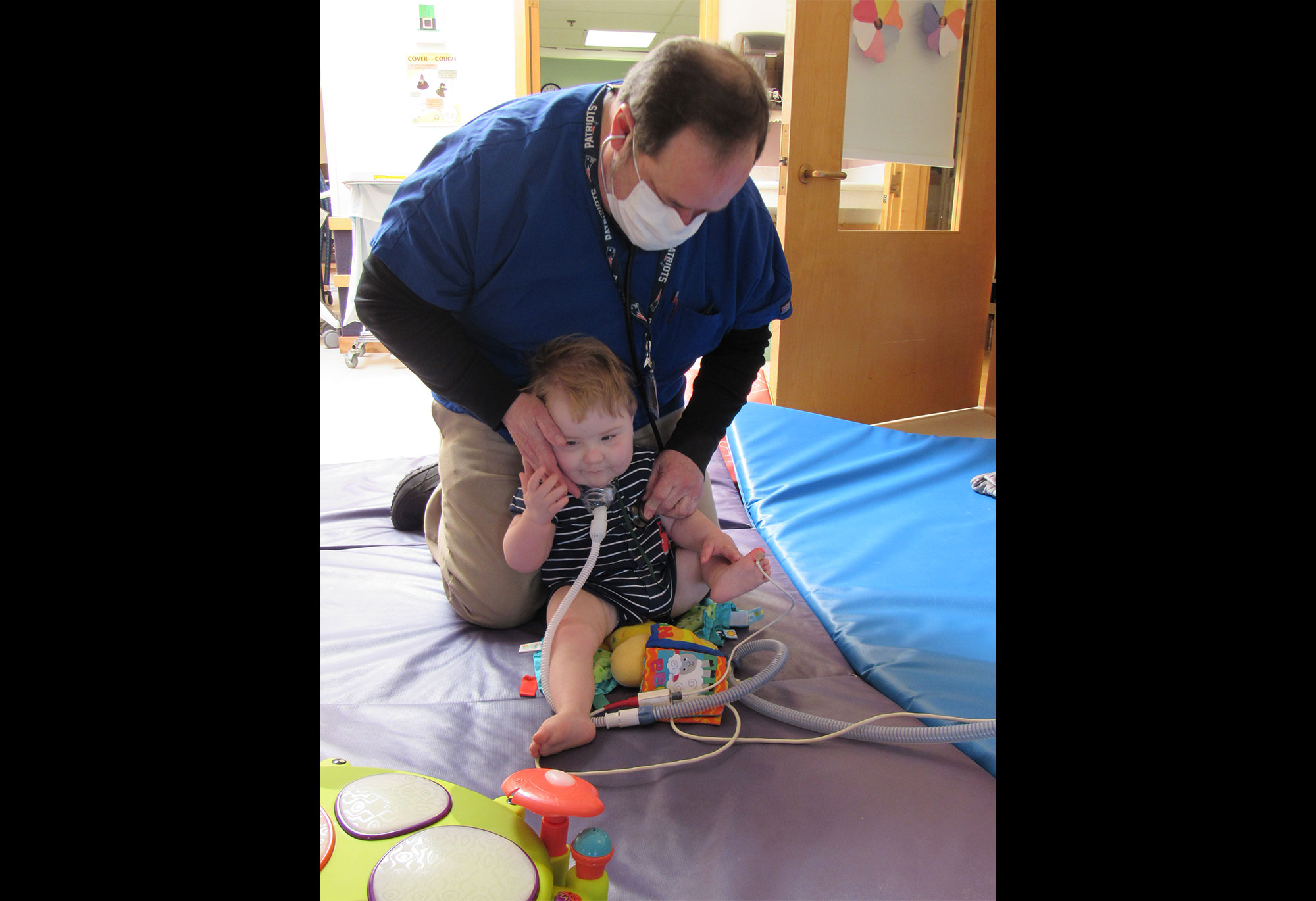
Cedarcrest Center for Children with Disabilities
Cedarcrest Center for Children with Disabilities in Keene enacted visitor restrictions for more than three months to anyone but staff, a federal requirement that was difficult for the organization and for the children it cares for.
“We were so cut off from the world,” said CEO Cathy Gray. “It was very different and unnerving, but everybody adapted and our mission was to keep the children healthy.”
Twenty children live at the center as in-patient residents. Some are on ventilators. Others have other breathing aids or compromised respiratory systems – so they are at high risk for illnesses including COVID-19. Their families stayed connected as best they could, through video conferencing and phone calls.
From March until mid-July, Cedarcrest also suspended short-term stays for children – stays that help ease stress on families.
The Center used video links for some services and remote learning for its day students, a challenging task for those with significant developmental disabilities. For day education students, staff provided families with resources so they could carry on at home. Some families joined daily school activities by video link. Day students were welcomed back in early July.
Behind the scenes, throughout the early months of the COVID-19 pandemic, some administrative staff worked from home, maintaining required electronic medical records and staying in touch with families.
The Foundation released payments of a multi-year operating grant early and awarded an additional grant that helped purchase secure laptops for staff working at home.
Aside from a concern early on when a couple of children had fevers (they quickly tested negative for COVID), the round-the-clock care for children has continued seamlessly.
“Fortunately, for the children, their day-to-day has not been affected, other than all of a sudden everybody’s got masks on and they are not seeing their families as often,” Gray said.
Despite dealing with the pandemic’s effects on their own lives, the staff has been staying grounded at work by focusing on the children who depend on them.
“They were interacting with the children, providing care, singing a song, playing a game,” Gray said. “Everybody knew the world was far different, but I think that definitely helped.”
Northeast Deaf and Hard of Hearing Services
At Northeast Deaf and Hard of Hearing Services, communication is their business – a business that’s been very difficult since face-to-face encounters ended in the spring and face masks became necessary.
Executive Director Susan Wolf-Downes said masks obviously make it impossible for deaf or hard of hearing people to read lips – so many hospitals, hearing interpreters and her organization have a supply of masks with transparent “windows” over the mouth area.
But lip-reading with face masks was among the least of NDHHS’s problems. With daily life suspended, calls for referrals or interpreter services that the organization provides halted – along with the income those calls brought to support the work.
“That was really frightening. It was like the whole world stopped,” Wolf-Downes said.
Those calls normally would come from doctors’ offices, courts, vocational rehabilitation programs, schools (for meetings or parent conferences), community groups, businesses (for presentations or training), even from people needing an interpreter to interact with a car mechanic.
Some schools requested help providing remote lessons to deaf and hard of hearing students, which involved getting information to parents and helping them get video access, with interpreters.
“It took some serious thinking and a lot of mind-stretching, but we are not the type to just say ‘Oh this can’t happen, because there is no ‘can’t.’ Kids need access and that’s what we are committed to,” Wolf-Downes said.
NDHHS maintained its Emergency Medical Interpreter Service Program, providing interpreters for five hospitals. The program ran with remote video services for several months, until interpreters were allowed back into hospitals.
The organization also works as a clearinghouse to make sure that people who are deaf and hard of hearing receive the latest COVID information. For many reasons, some deaf people cannot read captioning on TV, if there is captioning at all. Some were mainstreamed in school or did not receive early intervention programs, Wolf-Downes said. And while it’s very helpful to have an interpreter signing Gov. Chris Sununu’s COVID updates, not everyone has the opportunity or ability to watch.
Wolf-Downes said many people in the deaf community are hunkered down at home, including children who depend on some in-home early intervention programs that were suspended in the spring. Some families are using Zoom, but a number have no internet access, leaving their kids with no expert instruction.
“There are some parents who actually have no communication with their children at all,” Wolf-Downes said. “When their parents are talking to their siblings, and not talking to them, they are really lost in their own homes. It’s a nightmare to think about.”
Aside from isolation, behavioral problems increase when there is no communication.
Observing how pandemic restrictions have affected children has prompted NDHHS to plan new programs for life after COVID, including one called “Making Connections: Teens Like Me,” for deaf or hard of hearing teens.
“Often these children have never met another student with hearing loss or with cochlear implants or who is deaf and blind,” Wolf-Downes said. “They are isolated often, then they graduate and don’t have a community to go to.
“We are not required to provide that service, and we don’t get state funding for it, but it is something we are committed to doing,” she said.
Krempels Center
Krempels Center, in Portsmouth, works to improve the lives of people with brain injury by helping their members build skills in everything from communications to cooking, with support to boost their emotional and physical wellness.
When Krempels Center quickly moved programs online in the spring, not all members could take part because of various technical or physical challenges. But when it resumes regular programming, Krempels Center will be able to welcome back those members at its in-person programs, and continue to reach many more who now can participate online.
Brain-injury survivors have already endured significant unexpected challenges and, often, isolation. The public-health crisis has added more of both.
“We didn’t want our members to have the loss of our program where they already had experienced something so traumatic,” said Executive Director Lisa Couture. “How awful if we really had to completely disrupt these services where they are actually feeling hopeful again about what their life can be.”
Krempels Center typically closes for a break during the third week of March – just as the pandemic fallout hit. So this year, instead of taking a break, Krempels staff shifted into high gear and implemented fundamental changes, quickly. Over several days, they converted their programs online, then reached out to 100 currently or recently enrolled brain-injury survivors to inform them and gauge what help they might need to participate.
By the end of that week, many brain-injury survivors were taking part in pilot online programs. The virtual programs quickly attracted about 70 percent of the normal attendance.
While disappointed that new barriers prevent some members from participating online, she is overjoyed that technology has eliminated a troubling old barrier – lack of transportation or long, tiring drives to Portsmouth that limited or prevented participation for many others.
Pre-COVID, the parents of one member from Keene drove him to Portsmouth once a week – a four-hour round-trip. Now, he participates independently, online, three days a week.
Couture said virtual offerings have opened possibilities to people all over state.
“We are seeing this as the opportunity we have been waiting for,” she said, “which is to be able to serve folks with no geographic barriers.
“I’m practically in tears right now talking about it,” she said. “I feel so happy we’ve been able to do this and know the impact we’ve had and seeing those same folks who are so joyfully connecting with their peers in our programming instead of being home alone, isolated.”
Couture said it wouldn’t have happened without philanthropic help to make up for lost donations and fundraisers.
“That allowed us to focus where we needed to focus, which was on making sure we could keep offering meaningful services,” she said.
Nonprofits need help more than ever to sustain operations and respond to community need. Please consider giving to support their critical missions. If you are a fund-holder at the Charitable Foundation and would like to use your fund to address increased community needs during this time, please call 1-800-464-6641 and choose option three for donor services.